Boston Eczema Dermatologist
Jump To

Eczema is a broad term for a number of skin conditions that shows up as dry, irritated and very itchy skin. Another word for eczema is dermatitis. There are many different types of eczema or dermatitis. Some of the most common types of eczema include: atopic dermatitis, allergic contact dermatitis, irritant dermatitis and nummular dermatitis.
Eczema Symptoms
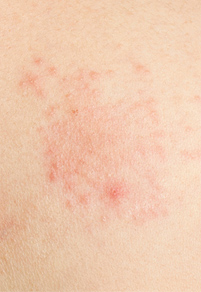
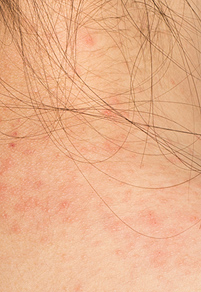
Patients with eczema experience dry, itchy skin. Eczema can occur on any part of the body. With a specific type of eczema known as atopic dermatitis, it most commonly affects the inner elbows and the backs of the knees. Irritant dermatitis, another type of eczema, is often seen on the hands. Eczema can be found in any area of the body, even the eyelids, scalp and groin can have eczema.
Eczema is often very itchy and patient will describe dry, red, cracked or flaking skin. Some say that their skin even burns.
Types of Eczema
*Important note: Eczema is a group of skin conditions that cause inflamed skin. Below are just a few of the different types of eczema.
Atopic Dermatitis
Atopic dermatitis is the most common type of eczema and usually starts in childhood. It is estimated that 1 in 10 Americans suffer from atopic dermatitis. It is characterized by dry, sensitive skin that becomes red and itchy. Atopic dermatitis can be challenging to manage because it can have many different triggers. Treatment options include avoiding triggers, using moisturizers to hydrate the skin, and taking medication.
Contact Dermatitis
Contact dermatitis occurs when the skin comes into contact with an irritant such as a chemical, poison ivy, or nickel. The symptoms appear within 24-48 hours after exposure and include itching, redness, swelling, and blisters. Treatment involves identifying the trigger and avoiding it if possible. It is imperative to see a board-certified dermatologist to treat contact dermatitis as quickly as possible.
Dyshidrotic Eczema
Dyshidrotic eczema is a type of eczema that affects the hands and feet. It is characterized by small blisters that itch and can be painful. The blisters typically occur on the palms of the hands or soles of the feet and can last for several weeks. Treatments can involve managing stress levels (as stress can worsen symptoms), using moisturizers to keep the skin hydrated and protected, and/or corticosteroids to reduce inflammation.
The Causes of Eczema
Most commonly, eczema is hereditary in nature. Many people believe that certain genes may cause people to have extra sensitive skin that can lead to eczema.
Some types of eczema are more common in people who have seasonal allergies and/or asthma. This type of eczema, known as atopic dermatitis, most often begins in childhood but can develop in adults too. Other types of eczema occur when the skin is overly sensitive to things that touch the skin such as cosmetics, preservatives and fragrance. Skin contact with substances that may cause irritation like wool, soaps, and synthetic fibers can also cause eczema. Allergy testing, known as patch testing, can be done to see if a patient has a sensitivity to something that is touching the skin.
Many types of eczema show up for reasons that we don’t understand. Eczema can worsen during certain seasons, most often in the winter.
Moreover, other factors such as stress, heat, sweat, food allergies and dry skin can also trigger eczema. Some kinds of food – for instance, nuts and dairy products – may trigger symptoms. Women may be affected with eczema during pregnancy or menstruation, as their hormonal levels change at this time.
It should be noted that eczema is not contagious. It does not spread by contact with affected people.
Eczema Dermatologist Treatment Options
Those with eczema should use gentle soaps and plenty of moisturizers. Dermatologists can prescribe different creams and pills that can soothe and repair the skin. The most commonly prescribed types of creams for eczema are steroid creams. Steroid creams can be very effective but they should not always be used on certain body parts and sometimes their use should be limited in duration. You should follow the instructions given to you for use of your steroid cream. Other types of creams prescribed for eczema treatment include: tacrolimus (Protopic ®), pimecrolimus (Elidel®) and crisaborole (Eucrisa®). For more severe cases of eczema certain pills can be given to improve the skin. For patients with the type of eczema known as atopic dermatitis, a shot called dupilumab (Dupixent®) can be effective to help the skin.
Therapies and lifestyle changes also go a long way in calming the symptoms of eczema. Because stress is also a cause, relaxing activities like yoga, breathing exercises, meditating and listening to music can be helpful. A warm bath and a good sleep can be quite effective, and some patients turn to alternative treatments such as acupuncture.
Call or contact our Boston location or schedule your consultation with one of our board-certified dermatologists, led by Dr. Emmy Graber.
Learn more about eczema and how to treat it at the American Academy of Dermatology: AAD Eczema
Eczema Dermatologist FAQs
Is eczema contagious?
No, eczema is not contagious. It is a non-infectious skin condition caused by various factors, such as genetics, environment, and certain substances. People with eczema usually cannot keep the moisture in their skin, leading to inflammation and irritation. Eczema can be triggered by stress and other environmental factors.
What are the most common triggers?
Common eczema triggers vary from person to person. Still, some of the most common include certain fabrics such as wool or synthetic fibers, soaps and detergents, exposure to water, heat, cold temperatures or humidity, pollen or pet dander, certain foods such as dairy products and eggs, stress, and emotional changes.
Can eczema be cured?
Eczema cannot be cured, but it can be managed with the right treatment plan and lifestyle changes. It is important to work closely with your dermatologist to develop an eczema management plan.
Is eczema the same as psoriasis?
No, eczema and psoriasis are two different skin conditions. They have many similarities, but there are also key differences. Eczema is a general term for a group of conditions that cause the skin to become inflamed or irritated. Psoriasis is caused by an overactive immune system that triggers skin cells to grow too quickly. Psoriasis also typically causes red, scaly patches that are thicker and more persistent than eczema. It is important to see a board-certified dermatologist for an accurate diagnosis and treatment plan for either condition.